![]()
Techniques in cell biology
Immunotechniques
Radioimmunoassay (RIA)
- One of the most sensitive techniques for detecting antigen or antibody is radioimmunoassay (RIA).
- The technique was first developed in 1960 by two endocrinologists, S.A. Berson and Rosalyn Yalow, to determine levels of insulin-anti-insulin complexes in diabetics.
- Although their technique encountered some skepticism, it soon proved its value for measuring hormones, serum proteins, drugs, and vitamins at concentrations of 0.001 micrograms per milliliter or less.
- In 1977, some years after Berson’s death, the significance of the technique was acknowledged by the award of a Nobel Prize to Yalow.
- The Principle of RIA involves competitive binding of radiolabeled antigen and unlabeled antigen to a high-affinity antibody.
- The labeled antigen is mixed with antibody at a concentration that saturates the antigen-binding sites of the antibody.
- Then test samples of unlabeled antigen of unknown concentration are added in progressively larger amounts.
- The antibody does not distinguish labeled from unlabeled antigen, so the two kinds of antigen compete for available binding sites on the antibody.
- As the concentration of unlabeled antigen increases, more labeled antigen will be displaced from the binding sites.
- The decrease in the amount of radio labeled antigen bound to specific antibody in the presence of the test sample is measured in order to determine the amount of antigen present in the test sample.
- The antigen is generally labeled with a gamma-emitting isotope such as 125I, but beta-emitting isotopes such as tritium (3H) are also routinely used as labels.
- The radio labeled antigen is part of the assay mixture; the test sample may be a complex mixture, such as serum or other body fluids, that contains the unlabeled antigen.
- The first step in setting up an RIA is to determine the amount of antibody needed to bind 50% to 70% of a fixed quantity of radioactive antigen in the assay mixture.
- This ratio of antibody to Ag* is chosen to ensure that the number of epitopes presented by the labeled antigen always exceeds the total number of antibody binding sites.
- Consequently, unlabeled antigen added to the sample mixture will compete with radio labeled antigen for the limited supply of antibody.
- Even a small amount of unlabeled antigen added to the assay mixture of labeled antigen and antibody will cause a decrease in the amount of radioactive antigen bound, and this decrease will be proportional to the amount of unlabeled antigen added.
- To determine the amount of labeled antigen bound, the Ag-Ab complex is precipitated to separate it from free antigen (antigen not bound to antibody), and the radioactivity in the precipitate is measured.
- A standard curve can be generated using unlabeled antigen samples of known concentration (in place of the test sample), and from this plot the amount of antigen in the test mixture may be precisely determined.
- Several methods have been developed for separating bound antigen from free antigen in RIA. One method involves precipitating Ag-Ab complexes with a secondary anti-isotope antiserum.

- For example, if the Ag-Ab complex contains rabbit IgG antibody, then goat anti-rabbit IgG will bind to the rabbit IgG and precipitate the complex.
- Another method makes use of the fact that protein A of Staphylococcus aureus has high affinity for IgG.
- If the Ag-Ab complex contains an IgG antibody, the complex can be precipitated by mixing with formalin-killed S. aureus.
- After removal of the complex by either of these methods, the amount of free labeled antigen remaining in the supernatant can be measured in a radiation counter; subtracting this value from the total amount of labeled antigen added yields the amount of labeled antigen bound.
- Various solid-phase RIAs have been developed that make it easier to separate the Ag-Ab complex from the unbound antigen.
- In some cases, the antibody is covalently cross-linked to Sepharose beads.
- The amount of radiolabeled antigen bound to the beads can be measured after the beads have been centrifuged and washed.
- Alternatively, the antibody can be immobilized on polystyrene or poly-vinyl chloride wells and the amount of free labeled antigen in the supernatant can be determined in a radiation counter.
- In another approach, the antibody is immobilized on the walls of microtiter wells and the amount of bound antigen determined.
- Because the procedure requires only small amounts of sample and can be conducted in small 96-well microtiter plates (slightly larger than a 3 × 5 card), this procedure is well suited for determining the concentration of a particular antigen in large numbers of samples.
- For example, a microtiter RIA has been widely used to screen for donor blood and has sharply reduced the incidence of hepatitis B infections in recipients of blood transfusions.
ELISA
- Enzyme-Linked Immunosorbent assay, commonly known as ELISA (or EIA), is similar in principle to RIA but depends on an enzyme rather than a radioactive label.
- An enzyme conjugated with an antibody reacts with a colorless substrate to generate a colored reaction product.
- Such a substrate is called a chromogenic substrate.
- A number of enzymes have been employed for ELISA, including alkaline phosphatase, horseradish peroxidase, and b-galactosidase.
- These assays match the sensitivity of RIAs and have the advantage of beings safer and less costly.
- There are numerous variants of ELISA
- A number of variations of ELISA have been developed, allowing qualitative detection or quantitative measurement of either antigen or antibody.
- Each type of ELISA can be used qualitatively to detect the presence of antibody or antigen.
- Alternatively, a standard curve based on known concentrations of antibody or antigen is prepared, from which the unknown concentration of a sample can be determined.
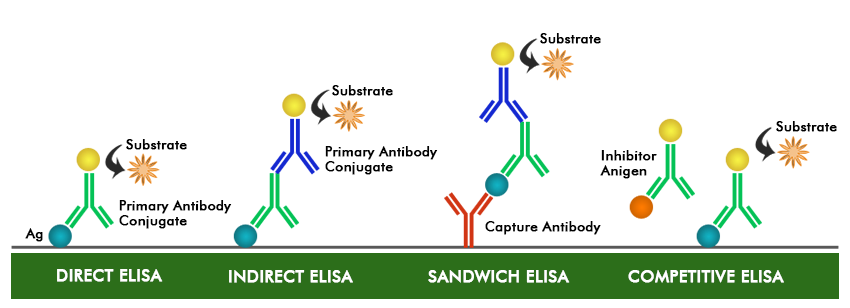
Indirect ELISA
- Antibody can be detected or quantitatively determined with an indirect ELISA.
- Serum or some other sample containing primary antibody (Ab1) is added to an antigen coated microtiter well and allowed to react with the antigen attached to the well.
- After any free Ab1 is washed away, the presence of antibody bound to the antigen is detected by adding an enzyme-conjugated secondary antibody (Ab2) that binds to the primary antibody.
- Any free Ab2 is then washed away, and a substrate for the enzyme is added.
- The amount of colored reaction product that forms is measured by specialized spectrophotometric plate readers, which can measured the absorbance of all of the wells of a 96-well plate in seconds.
- Indirect ELISA is the method of choice to detect the presence of serum antibodies against human immunodeficiency virus (HIV), the causative agent of AIDS.
- In this assay, recombinant envelope and core proteins of HIV are adsorbed as solid-phase antigens to microtiter wells. Individuals infected with HIV will produce serum antibodies to epitopes on these viral proteins. Generally, serum antibodies to HIV can be detected by indirect ELISA.
Sandwich ELISA
- Antigen can be detected or measured by a sandwich ELISA.
- In this technique, the antibody (rather than the antigen) is immobilized on a microtiter well.
- A sample containing antigen is added and allowed to react with the immobilized antibody.
- After the well is washed, a second enzyme-linked antibody specific for a different epitope on the antigen is added and allowed to react with the bound antigen.
- After any free second antibody is removed by washing, substrate is added, and the colored reaction product is measured.
Competitive ELISA
- Another variation for measuring amounts of antigen is competitive ELISA. In this technique, antibody is first incubated in solution with a sample containing antigen.
- The antigen antibody mixture is then added to an antigen coated microtiter well.
- The more antigen present in the sample, the less free antibody will be available to bind to the antigen-coated well.
- Addition of an enzyme-conjugated secondary antibody (Ab2) specific for the isotype of the primary antibody can be used to determine the amount of primary antibody bound to the well, as in an indirect ELISA. In the competitive assay, however, then higher the concentration of antigen in the original sample, the lower the absorbance.